Some suffer from depression. Others struggle with walking. Over half are women, and nearly 50% are from racial and ethnic minority groups. Approximately 40% come from households earning less than $50,000 per year. And they all have one thing in common.
All are users of telehealth, a commonsense healthcare reform that allows patients to access medical care from the comfort of their own home using a computer, smartphone, or landline phone, according to a new Goldwater Institute report. In fact, more than 20 percent of households in the Phoenix area are taking advantage of telehealth, all made possible by a new Goldwater Institute law enacted in 2021. As the report shows, that law is expanding services to some of the most vulnerable and under-resourced populations in the Phoenix area, including elderly residents, lower-income households, Black and Hispanic communities, and those who struggle with mental and physical health challenges.
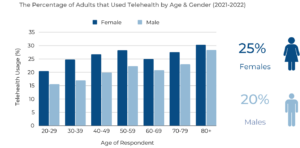
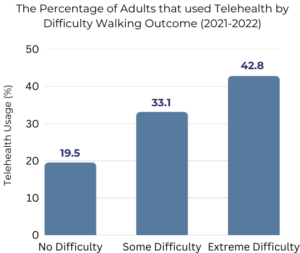
According to the report, one of the strongest predictors for telehealth utilization was difficulty walking, a factor closely associated with aging. Adults who reported extreme difficulty walking were over two times more likely to utilize telehealth compared to their counterparts who reported no physical challenges. Considering that by 2035, older adults will outnumber children, telehealth could play a critical role in allowing older individuals to age in place, particularly in Arizona’s rural areas—like La Paz, Yavapai, and Mohave counties, where more than 30% of their population is 65 years or older.
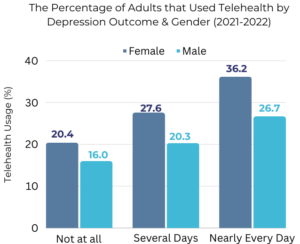
The second-strongest predictor for telehealth utilization in the Phoenix area was depression. As depression worsened, telehealth utilization increased for males and females across the board. Meanwhile, a 2021 national analysis showed that “Psychiatry and Substance Use Disorder Treatment” had the highest telehealth penetration compared to all other healthcare specialties—suggesting this arena of telehealth is extremely vital. This is particularly true for states that are facing extreme physician shortages—states like Arizona, which is almost last in the nation for the rate of availability of mental healthcare providers. Other benefits of comprehensive telehealth legislation in the mental health arena include: 1) decreasing stigma by removing the in-person care requirement, 2) increasing access for people in rural areas, 3) lowering the number of emergency room visits, and 4) addressing some of the devastating consequences related to mental illness, such as homelessness, overdoses, and suicide.
Telehealth overcomes one of the most significant obstacles for these populations: transportation—or just gaining entry into the healthcare system. Some researchers hypothesize that bringing care to where the patient is located has major benefits for communities that may mistrust in-person care, face transportation barriers, have difficulty taking time off from work, or struggle with physical infirmities that leave them homebound.
While some states, like Arizona, have recognized the groundbreaking potential of telehealth flexibilities and created permanent and comprehensive reforms, many more states have jumped off the telehealth cliff or have only made minor adjustments to their laws.
One major aspect of Arizona’s telehealth legislation is interstate telemedicine—or allowing out-of-state providers to practice medicine without having to jump through time-consuming hoops to obtain an in-state license, which takes at least a two-month wait, according to the American Medical Association.
Allowing providers to easily practice across state lines is a no-brainer. It improves accessibility, lowers appointment wait times, increases the number of specialty providers, and contributes to a more diverse pool of doctors who can then be more representative of the populations they serve. Apart from a few exceptions, more than 60% of states require out-of-state healthcare providers to be fully licensed in their state to practice telemedicine, while only a handful of states have completely removed this barrier.
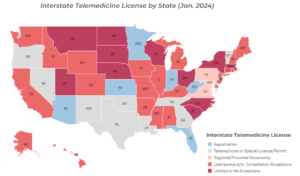
* Data obtained from the Federation of State Medical Boards (FSMB) and the Center for Connected Health Policy, January 28th, 2024. This map does not account for states that may have multiple exceptions and/or mechanisms to practice interstate telemedicine. Please refer to the FSMB for more detailed information .
*Telemedicine vs. telehealth – The map above uses the term telemedicine despite some states like Arizona that implement telehealth, meaning a broader range of healthcare services.
As the nation moves further away from the pandemic, states need to take a page out of the COVID-19 handbook and stop using outdated licensing laws as a barrier to entry for providers who are licensed and in good standing in other states. Significant demographic changes coupled with looming physician shortages require policymakers and health systems to make the right choice—the easy one—and open the door to 21st century healthcare.
There is no better way to improve health outcomes and holistically address accessibility than by bringing care to where the individual is located. More states and lawmakers need to follow Arizona’s lead and make telehealth flexibilities that were once temporary 100% permanent.
Read the full report here.














